Admin
Admin Heterogeneity in hepatitis C treatment prescribing and uptake in Australia: a geospatial analysis of a year of unrestricted treatment access
| Author List |
|---|
| Nick Scott |
| Samuel W Hainsworth |
| Rachel Sacks-Davis |
| Alisa Pedrana |
| Joseph Doyle |
| Amanda Wade |
| Margaret Hellard |
Abstract
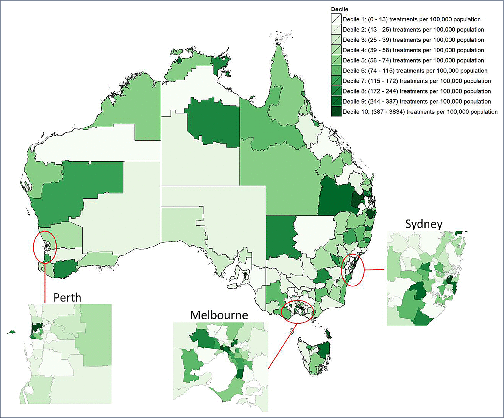
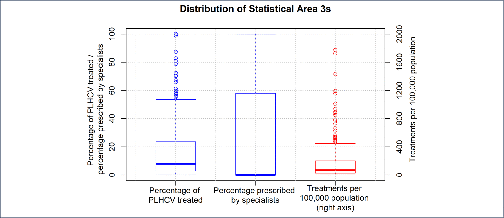
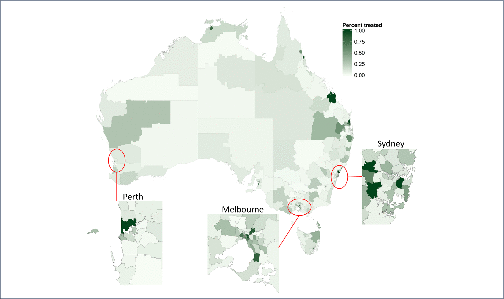
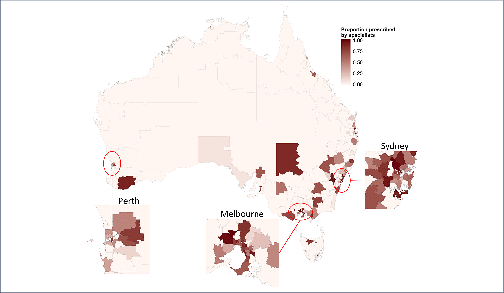
Background and aim: Direct-acting antiviral (DAA) treatments became available for all people living with hepatitis C virus (HCV) in Australia in March 2016. We assess variations in treatment rates and prescribing patterns across Australia‘s 338 Statistical Area 3 (SA3) geographical units. Methods: Geocoded DAA treatment initiation data were analysed for the period 1 March 2016 to 30 June 2017. Regression models tested associations between the population demographics and healthcare service coverage of geographical areas and (a) their treatment rates; and (b) the proportion of prescriptions written by specialists compared to non-specialists. Results: Across the 320 areas (95%) recording treatments, a median 76 (interquartile range [IQR] 35–207, range 4–3834) per 100,000 were initiated, corresponding to an estimated median 7.9% (IQR 2.9–23.6%, range 0–100%) treatment uptake. Major cities, areas of socioeconomic advantage and areas with lower proportions of the population born overseas had the highest per capita treatment rates. Non-specialists prescribed 46% (20,323/44,382) of treatment initiations. Prescriptions were written by non-specialists only in 163 areas (51%), while in other areas a median 40.0% (IQR 21.8–62.5%) of prescriptions were written by non-specialists. Non-specialist prescribing was higher in regional areas, as well as areas that had greater proportions of Indigenous Australians. Conclusions: High national-level treatment uptake of 20% in Australia masks underlying health system limitations; more than half of geographical areas may have treated less than 8% of people living with HCV. Areas of socioeconomic disadvantage and areas with a higher proportion of the population born overseas may need targeting with interventions to improve treatment uptake.
Published
Article Category
Hepatitis C (HCV)
Article Type
Original research
Posted Date
21-03-2018